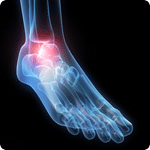
Heel Spurs
What Causes Heel Spurs?
The calcaneus is the largest of the 26 bones of the foot. Heel spurs occur when calcium—a mineral found throughout the body that helps your bones, muscles and cells work properly—builds up on the bottom of this bone. This buildup of calcium usually forms when the plantar fascia pulls away from the heel, which takes place gradually over a period of time. This is why heel spurs are commonly seen in patients with plantar fasciitis and the two conditions are linked. A heel spur can also develop on the back of the heel, and these types of spurs are associated with the condition Achilles tendonitis.
Heel spurs typically develop from putting too much strain on the muscles and ligaments of the feet and stretching them too far. They can occur in individuals of all ages, but are most common in middle-aged athletes involved in sports with lots of running and jumping. These physical activities put significant stress on the feet and make them more prone to injury. Individuals with an abnormal gait (walking style) or with improper foot structure (such as flat foot or high arches) are also at risk for heel spurs. Spending too much time on your feet, being overweight and wearing improper footwear—such as high heels, sandals or poor-fitting shoes—on a regular basis can add to this risk as well.
What are the Symptoms?
Although about 70% of patients with plantar fasciitis also have a heel spur, only about half of patients with heel spurs actually feel any pain from it. In most cases, the heel spur itself is not thought to cause any symptoms, but the condition it's associated with. When patients do notice symptoms, they experience pain and tenderness. This can be felt either at the bottom of the foot if it's associated with plantar fasciitis or behind the heel if connected to Achilles tendonitis. Like plantar fasciitis, the pain may be more pronounced in the morning and can also get worse when putting too much pressure on the heel from activities like running or jumping.
What Can Be Done?
If you have a heel spur as identified by an x-ray but don’t have any symptoms, treatment may not be needed until any pain develops. Some patients will improve on their own after avoiding activities that aggravate the heel, but for pain that lasts for more than one month, you should see a medical professional like a physical therapist or podiatrist. He or she will perform a full-scale evaluation that includes a physical examination, an interview and some tests to assess your heel. An x-ray is needed to confirm the presence of a heel spur, but this will not usually change the course of treatment. Since the heel spur itself is not responsible for symptoms, the condition it’s associated with—plantar fasciitis or Achilles tendonitis—will be addressed instead.
For this reason, conservative (non-surgical) treatment is typically prescribed for most heel spurs, and 90% of patients improve significantly with this type of approach. On the other hand, if you don’t do anything, the heel spur will grow and become more painful. The following steps may provide pain relief associated with heel spurs:
Rest
Limit or stop participating in high-impact activities that put too much stress on the heels such as running or basketball.
Ice
Apply an ice pack or cold compress to the heel for 15-20 minutes, 3-4 times a day.
Foot Supports
Heel cups or wedges like the DonJoy Silicone Heel Cups absorb shock, provide cushioning and elevate the heel; a podiatrist will be able to provide additional guidance on foot supports and decide if orthotics are also needed.
New Shoes
If your shoes—especially those used for physical activity—are worn out, don't fit properly or don't provide enough support, you should replace them with an appropriate pair; go to a running specialty store or ask your podiatrist or physical therapist for assistance.
Physical therapy
These remedies should help you improve, but sometimes physical therapy will also be needed to assist your recovery. All programs vary, but treatment for heel spurs typically consists of:
Education and Activity Modification
Your physical therapist will help you find ways to avoid straining your feet during activities and instruct you to adjust your workout routine and possibly lose weight.
Passive Therapies
Your physical therapist may perform massage or manipulations, or use devices like ultrasound or ice/heat directly on your heel.
Stretching Exercises
Active exercises—meaning they are performed by the patient—for the heel and calves will increase flexibility of the affected areas.
Strengthening Exercises
These active exercises build back up the strength of the lower leg and foot muscles to stabilize the ankle and heel.
Injections
If symptoms continue to be bothersome, a corticosteroid injection may be recommended by your doctor. This is an anti-inflammatory medication that's injected directly into your heel to temporarily relieve pain for a few months.
Surgery
If you still don't improve after 9-12 months of aggressive conservative treatment, surgery may be considered. Discuss options with your doctor, but the most common surgical procedures used for heel spurs are plantar fascia release and removal of the spur.
Can Heel Spurs be Prevented?
Just like any other injury, there is no guaranteed way to prevent a heel spur from developing, but you can make some changes to reduce the chances. Prevention methods are similar to other heel conditions and include the following:
- Always wear well-fitting shoes with soles that absorb shock and supportive heels, and be sure to replace old shoes and wear appropriate shoes for all activities
- Avoid walking barefoot on hard surfaces
- Warm up and stretch—especially your feet and lower legs—before engaging in any type of exercise
- If you're overweight, losing weight will reduce your risk for heel spurs
- Pace yourself and take breaks when exercising, especially if you start to notice any pain in your heel
SUPPORT & PROTECTION FOR HEEL SPURS
View All Products for Heel Spurs
-
 $33.71On Sale 0% Off Save $0.00(61) ReviewsRevolutionary heel support that cushions and stabilizes with every step. Lightweight design delivers targeted compression and comfort all day long. Protect your ankle, reduce pain, and stay active without limits.
$33.71On Sale 0% Off Save $0.00(61) ReviewsRevolutionary heel support that cushions and stabilizes with every step. Lightweight design delivers targeted compression and comfort all day long. Protect your ankle, reduce pain, and stay active without limits.The Airheel Arch & Heel Support can be used to treat or prevent the following ankle injuries:
- Airheel Arch & Heel Support
- Achilles Tendonitis
-
 $43.89On Sale 0% Off Save $0.00Protect your heels with DonJoy® Silicone Heel Cups — designed for maximum shock absorption and heel pain relief. Ideal for plantar fasciitis and heel spurs, they provide cushioning and reduce pressure during every step. Stay comfortable and supported with trusted orthopedic heel protection.
$43.89On Sale 0% Off Save $0.00Protect your heels with DonJoy® Silicone Heel Cups — designed for maximum shock absorption and heel pain relief. Ideal for plantar fasciitis and heel spurs, they provide cushioning and reduce pressure during every step. Stay comfortable and supported with trusted orthopedic heel protection.